Laparoscopy
The laparoscopy is an important diagnostic test which
allows the physician to visualize the reproductive organs within the
pelvic cavity. It is performed as a hospital outpatient procedure
under general anesthesia. Two small incisions are made in the
abdomen, one at the belly button and one above the pubic bone (at
the pubic hair line).
In the laparoscopy, a small "telescope" is inserted
through one of the incisions and the surgical tools are passed, and
operated, through the other. The abdomen is filled with gas which
allows the physician to clearly view the surfaces of the internal
organs such as the ovaries, tubes, and uterus.
Many times our patients have already had one or more
laparoscopies by the time they seek specialist care. Laparoscopy for
the diagnosis and treatment of infertility should always be
performed by a reproductive specialist who has extensive training
and experience in microsurgery.
The incidence of complications from laparoscopy, such
as scarring or adhesions, may be less when a specialist performs the
laparoscopy. It is oftentimes possible to treat conditions, such as
endometriosis, during the diagnostic laparoscopy. The operating
surgeon must have the skills necessary to perform the complex
surgery that is often required.
Studies indicate that the presence of very small
amounts of endometriosis in the pelvic cavity can reduce IVF success
rates by creating a hostile inflammatory environment. The
reproductive surgeon must exercise painstaking care to remove all
endometriotic lesions.
 back
back
Post
Coital Fertility Test
The post coital fertility test, or "after
intercourse", test determines the ability of the sperm to survive in
the cervical mucus. The couple has intercourse at home and the
female comes to the office within 24 hours later. The cervical mucus
is examined and numerous "dead" or nonmoving sperm indicate there
may be an antibody problem.
Antibody reactions occur when the female's body
mistakes the sperm for invading pathogens and seeks to destroy them.
The male can also rarely produce antisperm antibodies.
 back
back
Hysterosalpingogram (HSG)
Infertility can result from blocked fallopian tubes
or an abnormally shaped uterus. The hysterosalpingogram ( HSG
)involves passing a small catheter through the cervix and injecting
dye into the uterus. The passage of the dye from the uterus through
the fallopian tubes and into the abdominal cavity is visualized by
x-ray.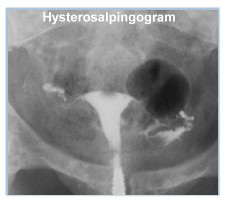
If the tubes are blocked, the dye cannot pass and
this is clearly seen on x-ray. Uterine polyps, fibroids, or
anatomical abnormalities are often visible in the HSG. Oftentimes a
hysterosonogram using contrast media is used to further evaluate the
uterus.
Interestingly, some women become pregnant after the
HSG. The procedure is not a "treatment" for infertility but forcing
the dye through the tubes may cause opening or removal of small
blockages.
Dr. Abou Abdallah has extensive experience conducting and
evaluating the HSG which he personally performs at the hospital.
 back
back
Hysteroscopy
The hysteroscopy allows the physician to visualize
the inside of the uterus. A small "telescope" is passed through the
vagina into the uterus. The uterus is filled with carbon dioxide gas
or special solutions causing it to expand. The physician can clearly
see the inside of the uterus and identify polyps, fibroids,
adhesions, or other structural abnormalities.
.
 back
back
Sonohysterogram
The sonohysterogram is used to evaluate the uterus
and we perform the procedure in our office. The uterus is filled and
expanded with saline solution, by passing a catheter through the
vagina. The vaginal probe is inserted into the vagina and used to
visualize the uterus via ultrasound. Abnormalities such as polyps
and fibroids can usually be seen.
The ultrasound is a valuable tool for evaluating the
ovaries, uterus, and other internal organs. The ultrasound uses
sound waves to generate images similar to x-ray without the
accompanying radiation.
 back
back
Vaginal Probe Ultrasound
The vaginal probe ultrasound is placed inside the
vagina and allows visualization of the ovaries, follicles, and
uterus. Patients undergo several
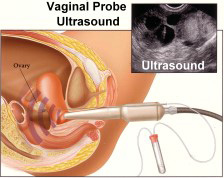 ultrasound
evaluations during drug stimulated ovulation cycles to monitor the
number and size of the follicles. These data are used to
individualize each patient's drug treatment protocol and help
determine when ovulation should be triggered. ultrasound
evaluations during drug stimulated ovulation cycles to monitor the
number and size of the follicles. These data are used to
individualize each patient's drug treatment protocol and help
determine when ovulation should be triggered.
Ultrasound is also used to measure the thickness of
the endometrium which indicates its readiness to accept and support
an embryo. Additionally, ultrasound can be useful in diagnosing
polyps and fibroids within the uterus, congenital malformations,
ovarian tumors, and documenting pregnancy.
 back
back
|

